
Brazilian research brings unprecedented information regarding the differential diagnosis between sporotrichosis and leishmaniasis
Article presents dermoscopic differences between sporotrichosis and leishmaniasis lesions
11/08/2023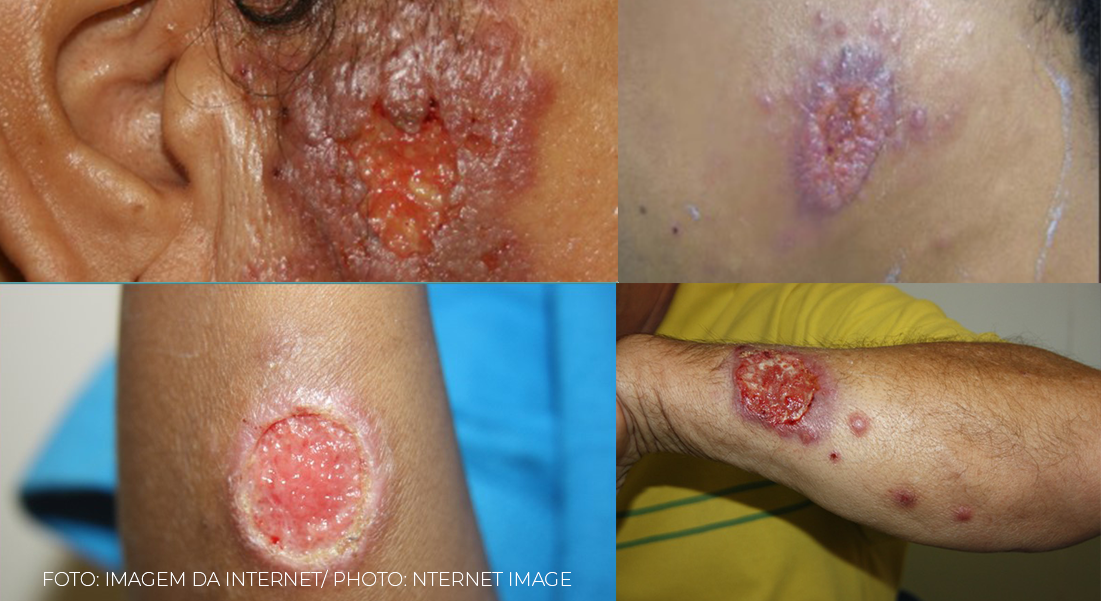
The first two images demonstrate how similar the two diseases can be. The third image is about sporotrichosis simulating leishmaniasis. And the last one, leishmaniasis with sporotrichoid aspect
Leishmaniasis and sporotrichosis are diseases that, although distinct in their causes and symptoms, can often be confused due to some clinical similarities. Both are infections that affect humans and animals, and their manifestations may vary according to the geographic region and the patient’s immune system. They can cause skin lesions such as ulcers, nodules, plaques or verrucous lesions. The correct diagnosis can be difficult without performing specific laboratory tests. Evolutionary aspects and epidemiological history can contribute to the proper diagnosis as well as the presentation of scarring aspects.
In histopathology there can also be confusion. Both are granulomatous diseases in which the presence of the etiological agents (amastigotes or fungal structures) often cannot be observed, and when present they can be confused.
To differentiate the two diseases, which are confused from a clinical and histopathological point of view, Dr. Marcelo Rosandiski Lyra supervised a master’s thesis that sought to establish criteria that would help the dermatologist or infectologist, or another professional who masters the technique of dermoscopy, to differentiate sporotrichosis and leishmaniasis. The article entitled “ Description of the dermatoscopic features observed in sporotrichosis and American cutaneous leishmaniasis in a reference center in Rio de Janeiro, Brazil ”, which has been accepted and is being printed, will be published in the next issue of Anais Brasileiros de Dermatologia.
To learn more about the subject, the press office of the Brazilian Society of Tropical Medicine (SBMT) interviewed Dr. Marcelo Rosandiski Lyra, dermatologist at the Evandro Chagas National Institute of Infectology (INI/Fiocruz), who works in the leishmaniasis laboratory in Rio de Janeiro, where cases of sporotrichosis are very frequent and, according to him, he has received patients diagnosed with clinical suspicion of leishmaniasis when it comes to sporotrichosis.
Check the interview in full.
SBMT: Why is the differentiation between the two diseases, sporotrichosis and leishmaniasis, an important topic? Are the two common diseases in dermatology and infectology care?
Dr. Marcelo Rosandiski Lyra:Physicians generally associate sporotrichosis with ascending nodular lymphangitis; however, in about 30% of the cases of sporotrichosis, the lesions are unique (fixed form), on the other hand, leishmaniasis is usually related to the presence of the ulcer, but there can be a wide variety of presentations regarding the number and morphology of the lesions. The differentiation of the two diseases is very important because one can mimic the other, for example, some sporotrichosis lesions will have an ulcerated aspect similar to leishmaniasis. The most common characteristic of sporotrichosis is the presence of several gummy lesions that follow the lymphatic path. However, occasionally, patients with leishmaniasis can also simulate the sporotrichoid aspect, with nodules arising from the primary ulcerated or verrucous lesion. I.e,
Furthermore, both diseases coexist in certain regions, such as here in Rio de Janeiro, as well as in other regions of Brazil. Therefore, it is essential for the doctor to know how to differentiate between them. In Rio de Janeiro, it is especially important because the number of cases of sporotrichosis has increased exponentially in recent years and it is not uncommon for me to receive patients at the leishmaniasis clinic with this diagnostic suspicion, but which, in fact, are cases of sporotrichosis.
SBMT: How does dermoscopy add to the traditional clinical examination?
Dr. Marcelo Rosandiski Lyra: Dermoscopy is an image exam that complements the clinical exam, using a manual device to amplify morphological structures present in the layers of the skin that are not visible to the naked eye. It is not a magnifying glass, as the exam allows you to see beyond the surface of the skin. This method is now widely used by dermatologists, but any physician with training is able to recognize and make good use of dermoscopy. The recognition of these structures that we find in the skin allows the doctor to detect patterns that can help in the differential diagnosis between clinically similar diseases, in this case, sporotrichosis and leishmaniasis.
SBMT: Did the findings reported in your study contribute to the clinical differentiation between the two diseases?
Dr. Marcelo Rosandiski Lyra:I believe that the study’s findings shed light on an understudied subject. Almost all studies that used dermoscopy to assess leishmaniasis were from patients from the Old World. And it is worth remembering that the disease we have in Brazil, in Latin America, American Tegumentary Leishmaniasis, is different from that observed in Old World countries, such as Europe, Africa and Asia. In relation to sporotrichosis, reports were even rarer. At the time of the study, we did not see four publications with case reports of dermoscopy and sporotrichosis. In this master’s thesis, 74 leishmaniasis lesions and 24 sporotrichosis lesions were evaluated, in three different moments, before, during and after treatment. We describe the dermoscopic findings in these three moments, which allowed us to observe some dermoscopic structures, until then, not described for these two diseases. But perhaps the most relevant contribution is not the finding of a single structure in isolation, but rather the recognition of a global dermoscopic pattern, that is, a pattern of how these structures are organized in sporotrichosis and leishmaniasis. And how this pattern tends to change evolutionarily, assuming characteristics peculiar to each of these diseases. This was perhaps the greatest contribution of the study. And how this pattern tends to change evolutionarily, assuming characteristics peculiar to each of these diseases. This was perhaps the greatest contribution of the study. And how this pattern tends to change evolutionarily, assuming characteristics peculiar to each of these diseases. This was perhaps the greatest contribution of the study.
Recognition of the patterns of organization of these dermoscopic structures in leishmaniasis and sporotrichosis can help the physician to differentiate between the two diseases, which are very similar from a clinical point of view. This is important because the doctor who is going to treat the patient with sporotrichosis or leishmaniasis is not always in a large center where he has the possibility of performing skin biopsy, fungal culture, culture for leishmania, or has access to the molecular method. That is, even being in a very remote place, with the aid of a manual device, the correct interpretation of dermoscopic findings can help in making a more accurate decision regarding the diagnosis. I make it clear that the findings are not pathognomonic, the dermoscopic examination is a complementary diagnostic method and must be interpreted together with the clinic,
SBMT: Does the delay in diagnosis or an initially mistaken diagnosis bring what risks to patients?
Dr. Marcelo Rosandiski Lyra: It is clear that when the diagnosis of a disease that is treatable is delayed, this allows it to evolve and naturally bring complications that would not occur if the patient were treated more quickly. Dermoscopy contributes to a correct diagnosis in places where there are limited resources, little access to laboratory tests and, therefore, it can contribute to the decision making of a correct diagnosis.
SBMT: Are the current treatments for both diseases satisfactory? Considering the possibility of cure, convenience of using medications, among other factors?
Dr. Marcelo Rosandiski Lyra:The treatments available for leishmaniasis are far from ideal. The drugs used today are intramuscular or intravenous and are extremely toxic, they are hepatotoxic, nephrotoxic, cardiotoxic. For example, meglumine antimoniate, which is the cornerstone of the treatment of leishmaniasis, began to be used in 1912, that is, we are talking about a drug that has been used for over 100 years. Evolution in terms of treatment for leishmaniasis is still very slow. New alternatives have recently emerged, we have miltefosine, non-cardiotoxic and because it is for oral use it is an interesting option, but it also has its negative points, in addition to the high cost it is a teratogenic drug, that is, it can lead to fetal malformation. Another approach is to use the same remedies more rationally, for example,
With regard to sporotrichosis, itraconazole is the drug of first choice, relatively inexpensive and well tolerated. Another alternative, such as terbinafine, follows the same line, is not as expensive a treatment and is equally well tolerated by the patient. We also have saturated potassium iodide solution as an alternative. In general, I would say that sporotrichosis has a safer treatment in terms of toxicity than leishmaniasis, but it should be noted that these antifungals that are used to treat sporotrichosis were not developed for this purpose, but to treat other fungal diseases It is. Naturally, sporotrichosis ended up “piggybacking” on the development of these drugs.
SBMT: Can we say that the two diseases fit the list of neglected infectious diseases?
Dr. Marcelo Rosandiski Lyra:There is no doubt that leishmaniasis is a neglected disease, which affects poor people in developing countries, not arousing great interest in investments by the pharmaceutical industry in search of new drugs. That is, leishmaniasis does not give financial return to laboratories. Sporotrichosis, on the other hand, is a little different: although most of the population that has sporotrichosis is still poor people, it is related to certain activities and professions, such as veterinarians, who come into contact with cats, the main transmitters of the disease, and people who work in a forest or rural environment. Here in Rio de Janeiro, the disease mainly affects people who own or care for cats. Therefore, it is not a disease exclusively limited to the less favored income population.
SBMT: Would you like to add something?
Dr. Marcelo Rosandiski Lyra: I would like to thank you for the opportunity to publicize the work and remind you that it is not definitive in terms of clarification, the distinction between sporotrichosis and leishmaniasis, but dermoscopy is one more tool that the doctor can use use to help you diagnose between these two diseases that can be so similar. Dermoscopy today is practically only performed by dermatologists, but any doctor who is interested in the subject can learn to master the technique, just needing training in which he will learn to recognize, identify and classify the structures.
Know more:










