
Initial approach to respiratory syndrome in times of COVID-19
What healthcare professionals should be aware of during a pandemic
11/06/2020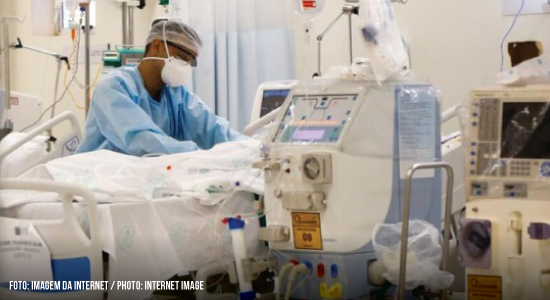
The dimension of the pandemic and its repercussions are felt at different levels of society, with a special impact on the dynamics of health services
Since the emergence of the first cases and the identification of the SARS-CoV-2 virus as a cause of severe acute respiratory syndrome (COVID-19) in January of this year in Hubei province, China, to the present day, with the declaration of a pandemic in March by the World Health Organization (WHO), it is estimated that there were more than 6.5 million cases and 386 thousand confirmed deaths from COVID-19. The dimension of the pandemic and its repercussions are felt at different levels of society, with a special impact on the dynamics of health services. Here we raise some points to assist professionals dealing with the care of suspected or confirmed patients in the initial phase.
One of the fundamental aspects of the epidemiological moment faced is related to control measures known to be effective, restricted at the moment to physical distance and the use of Personal Protective Equipment (PPE) suitable for health professionals. At first, with adherence to such measures, the guidelines focused on users only looking for health services with severe dyspnea and/or decompensation of underlying diseases, in an attempt both to restrict the circulation of people and to protect professionals and users from the risk of transmission on the way or in health services.
However, with the increase in the number of cases in several cities in the country, one of the aspects pointed out by several clinicians was that patients were arriving at very advanced stages of the disease. This is due to a combination of factors: 1. Fear of patients seeking health services for fear of becoming infected; 2. Guidance to only seek attention with pictures of severe dyspnea; 3. Absence of dyspnea even in patients with significant hypoxemia. The lack of perception of hypoxemia has been called “silent hypoxia” and its mechanism has not yet been fully elucidated, which may be due to damage to the surfactant-producing cells or changes in the center of perception of hypoxia in the central nervous system.
The first step is to consider the possibility of SARS-CoV-2 infection in patients experiencing respiratory symptoms, including cough, fever, shortness of breath, runny nose, anosmia, ageusia, in addition to diarrhea and other symptoms. Professionals attending patients with these symptoms should wear appropriate PPE including N95, mask, goggles and/or face shields, cloak and gloves. Although the attention and suspicion of COVID-19 are duly increased, clinicians should consider alternative diagnoses, such as infection by other respiratory agents (bacterial pneumonia, tuberculosis, among others), by arboviruses (Espirito Santo and Bahia face chikungunya epidemics, for example), in addition to other infectious and non-infectious conditions.
Next, it is important to assess the clinical condition to indicate either home isolation (if the patient is well), or whether the patient should be hospitalized or taken to a referral service. Thus, the initial assessment includes:
- Clinical evaluation of the patient – suspected or not of COVID-19?
- Testing/notification of the case (preferably with RT-PCR for virus detection).
- Classification of the case according to severity criteria.
- Conduct definition.
Among some of the most uncertain aspects of the approach to patients with COVID-19, is the definition of severity criteria. Being a recent disease, there are still many aspects to be studied and better defined.
Are there any early signs that the patient may get worse and needs to be hospitalized?
COVID-19 patients tend to complicate and deteriorate their clinical status between 7 and 14 days after the onset of symptoms. In diseases with a longer course, it is desirable to be able to identify signs of poor early prognosis, which can guide clinicians in the management of patients and modify the evolution of the disease. In dengue, for example, it was possible to establish warning signs and risk groups that, when well established in the routines of health services, substantially reduce complications and mortality by dengue. In the case of COVID-19, what can be evaluated?
We can define demographic aspects, clinical and laboratory signs of classification. The factors that have been associated with a worse prognosis include age over 65 years, male gender, presence of comorbidities and obesity. As for the clinical aspects, presence of dyspnea, cyanosis and hypoxemia (oxygen saturation below 95%). Regarding laboratory aspects, lymphopenia, thrombocytopenia, elevated neutrophil/lymphocyte ratio, C-reactive protein, elevated lactic dehydrogenase (DHL), elevated D-dimer, elevated cardiac troponin I and elevated interleukin 6 have been described as having a worse prognosis. However, none of these factors have yet been incorporated and validated for use in clinical practice, being almost restricted to the clinical approach and at the discretion of the professional. In a scenario of uncertainty and awaiting definitive studies, the service proposal is summarized in the table below.
Important to remember, there is no specific treatment against COVID-19 and what has an impact is quality clinical management, with critical support when necessary, which will be addressed in the next edition.











