
Vulnerability testing as a strategy to control COVID-19
Traditional infection control and public health strategies rely heavily on early detection of the disease to stem the spread
11/06/2020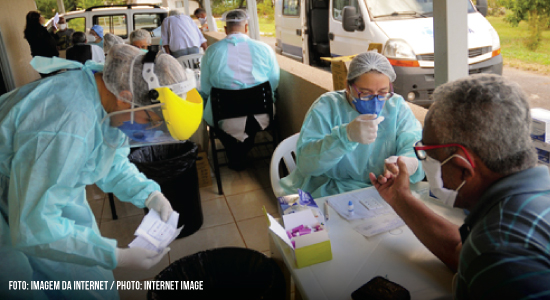
Asymptomatic individuals living or working in nursing homes will help control outbreaks and protect older patients who are at risk
Recent scientific studies indicate that up to 60% of COVID-19 transmissions occur through asymptomatic patients. Researchers argue that conducting large-scale tests to find and isolate asymptomatic cases, especially among healthcare professionals, who may inadvertently transmit the virus to colleagues or patients, is a vital strategy to curb the spread of the disease.
Dr. Monica Gandhi, Professor of Medicine and Associate Chief at the Division of HIV, Infectious Diseases, and Global Medicine, Director at the UCSF-Gladstone Center for AIDS Research (CFAR) and Medical Director at “Ward 86” HIV Clinic, San Francisco General Hospital, author of the article published in April in the New England Journal of Medicine entitled “Asymptomatic Transmission, the Achilles Heel of Current Strategies to Control COVID-19”, advocates adopting a new approach that expands testing COVID-19 to include asymptomatic people living or working in nursing environments. To her, symptom-based screening alone fails to detect a high proportion of infectious cases and is not sufficient to control transmission in closed environments, such as nursing homes. A new approach that expands the tests to include asymptomatic individuals living or working in nursing homes will help to control outbreaks and protect older patients, who are at risk of severe illness, she says.
Also, according to the professor, who is also holds a master’s degree in Public Health, mass testing of residents in nursing homes will allow adequate isolation and quarantine procedures. “We also expanded this recommendation to other situations of coexistence, such as pensions and prisons, closed mental health hospitals, shelters for homeless people and inpatients” she warns. In her opinion, the current test capacity must immediately increase for this strategy to be implemented. The strategies we recommend for conducting mass testing campaigns in vulnerable environments for residents and employees will require a significant increase in testing capacity, notes Dr. Gandhi
Another efficient and effective way to stem the spread of the new coronavirus is to track where people with COVID-19 are, including asymptomatic groups. However, Dr. Gandhi, who is also a medical director at the Gladstone AIDS Research Center, clarifies that in places like the United States, where the mass transmission of the community has already occurred, she doubts that everyone can be tested and traced. “That is why I recommend focusing on vulnerable groups in closed environments. I dont think its feasible to expect contact markers to be next to all infected patients, hoping to track all possible contacts to quarantine. The United States is the third most populous country on the planet, the period is arguably past in terms of using contact tracing to contain spread in the general population.
Asymptomatic patients make control of COVID-19 more difficult
An infected individual starts to show symptoms about five days after the infection, but there are people who always remain asymptomatic, they are those who do not perceive the virus and do not have serious conditions again, although they can transmit it to others. Dr. Gandhi points out that an asymptomatic person can be as contagious as a person with symptoms, as shown in small studies that demonstrate that viral loads in the nose and mouth among those who do not have symptoms are as high as those who have symptoms.
Regarding the spread of asymptomatic infection, the researcher explains that although there are some initial models of the percentage of infection spread by asymptomatic people (about 55%) versus symptomatic people, the data are still emerging. “However, we have certainly seen asymptomatic infection rates increase over time – initiated with 18% in Diamond Princess (without masks or caution); half at the start of a nursing home in Washington state; 53% in a mass testing campaign in the LatinX district of San Francisco; ~ 90% in a mass testing campaign at the largest homeless shelter in San Francisco; 96% of 3300 prisoners tested positive for SARS-Co-V in four Ohio prisons. Doctors around the world are reporting increasing rates of asymptomatic infection”, she laments.
The testing of asymptomatic individuals represents an important strategy because someone who can infect more susceptible individuals is removed from circulation. However, asymptomatic infection appears to be common and should continue to complicate efforts to control the pandemic. For Dr. Gandhi, asymptomatic infection can be both good and bad. For her, the problem is that the asymptomatic infection can still lead to transmission to other people. But, masking and other strategies can reduce this possibility. However, if higher rates of asymptomatic infection occur worldwide, this may be a good thing, this is preferable to a serious illness, she says. Still according to the professor, it may be that universal masking and other strategies are leading to exposures with lower inocula. Dr. Gandhi also highlights higher rates of exposure, as observed in antibody testing campaigns in Japan, without the unacceptable consequences of serious illnesses, can lead to greater immunity at the community level while the world awaits a vaccine.
According to the World Health Organization (WHO), the record of research on transmissions of asymptomatic and pre-symptomatic people indicates that:
- 6.4% of the 157 people monitored in research at the Center for Disease Control and Prevention (CDC) in the United States, on March 16 had been infected by pre-symptomatic patients. The transmission took place at an interval of one to three days before the symptoms manifested by the source patient;
- In China, asymptomatic patients were responsible for transmissions from 46% to 62% of cases, according to researchers at Columbia University, in the United States, in a study published on March 16 based on collected data and a metapopulation model;
- 48% of transmissions in Singapore and 62% in the city of Tianjin, China, originated from asymptomatic individuals, according to a study developed by Dutch and Belgian researchers, published on March 18
In January, 86% of cases in China, in Wuhan, were asymptomatic patients. And it is worth remembering that asymptomatic patients can transmit to others without imposing social distance and wearing masks in public. Finally, Dr. Gandhi notes that after an asymptomatic infection, the person may have antibodies against SARS-CoV-2 in the blood. “It is likely that, even after an asymptomatic infection, not just a symptomatic infection, the individual can obtain antibodies against SARS-CoV-2 in the blood”, she emphasizes. According to her, this would be a great advantage of asymptomatic infection (if the person is infected without showing signs of illness and then has immunity). “But more studies on this are still needed”, concludes the professor.










